We thank Paola from the bottom of our heart for sharing her story of her medical evacuation with us. We wish you all the best Paola!
Monday morning, 23 October.
I am sitting on the pavement outside my parents’ apartment in Rome, tears streaming down my face, head in hands. I’m supposed to be meeting my friend Anna at Piazza di Spagna in half an hour.
But I’m not sure I’ll make it. I feel unsteady. My chest feels tight. Come to think of it my jaw and upper arms feel tight too…
Deep breath, I tell myself. This is just stress. And no wonder I’m stressed. It’s less than a week since a close family member died: we were called to his bedside in Ireland from our home in Ghana three weeks ago, and spent his last two weeks with him. It was tough – indescribably tough – to watch him fade day by day. And after his funeral three days ago I came to visit my aging parents in Rome…my fourth or fifth visit this year? Too much all at once.
But I must pull myself together: this is supposed to be a fun morning: Anna and I are going to buy me a dress to wear to my son’s wedding in January. Retail therapy is just what I need before I fly back to Accra tomorrow. Another few deep breaths.
I call Anna. ‘I’m running late,’ I say, and explain the situation
‘Just take your time, go into a café, relax, have a coffee…’
And sure enough, the invisible clamp which is squeezing my chest gradually releases its grip. Half an hour later I feel ready to take the metro, if still a bit shaky, and a couple of hours later, exquisite new navy blue silk dress in hand, I am happily wandering around Trastevere with Anna, soaking in the heartwarming Roman autumn sunshine.
The following evening, I am in Accra.
Flash forwards five days to Sunday 29 October.
It’s been a relaxing, lazy day. I go to bed early, and am reading when a startlingly familiar feeling sweeps over me: tight chest, tight jaw, tight upper arms. Again, I think it’s just accumulated stress and fatigue. I call my husband, who comes upstairs, sits beside me, holds my hand, and says ‘Deep breaths, it’s been a tough few weeks, relax, we’ll get you checked out at WARA tomorrow.’ WARA, the West African Relief Association, is our clinic.
No alarm bells ring, although I have done several Red Cross courses over the years…I did them in order to be prepared in case there was an emergency with my husband: many of his family members have had heart problems. I never imagined I would be affected. I am fit: I practise yoga regularly and swim for half an hour almost every day; I am not overweight, have never smoked, eat healthily, and drink only moderately.
True, I have a classic ‘hyper’ personality. I have been taking medication to lower my blood pressure for about fifteen years, but have never really got it under control.
This second time, the tightness lasts an hour and a half, and I eventually get to sleep.
The next morning I go to WARA. My ECG is perfect. My blood pressure is rather high, but that’s to be expected under the circumstances, I tell myself. I send my husband a text message: ‘Phew, I’m fine!’ I still feel a little light-headed, but put it down to tiredness. The doctor takes a blood sample. ‘The first results will take half an hour,’ he says.
‘Okay, I’ll go shopping then come back for them.’
‘No, I’m sorry, you will do no such thing. You will sit quietly right here and wait. Chest pains are no joke.’
That’s when it hits me that this might be serious.
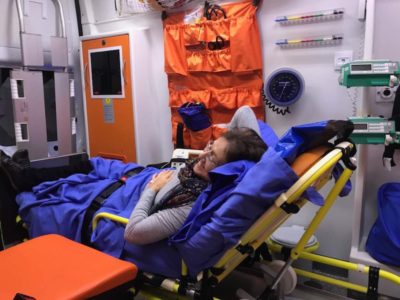
In the air ambulance
Half an hour later there’s a flurry of activity. I am told that high levels of troponins (enzymes I have never heard of) have been released into my blood and this indicates damage to my heart. My husband is called from his office and within minutes I am bundled into an ambulance.
‘Can I travel with her?’ my husband asks.
‘Well, you’d better follow in your own car, as we don’t know if she’s coming back,’ the Afrikaaner paramedic says in his thick accent. I don’t think he intends it with the meaning we interpret, but we giggle. At this stage my only feeling is one of apprehension: physically I feel fine, and chat and joke all the way to Korle-Bo, Ghana’s oldest government hospital.
At Korle-Bo I have another ECG and blood test, which confirm WARA’s findings. I see the chief cardiologist, who gives me a heart scan, which shows nothing untoward. I am admitted into a room and given blood thinners, statins and anticoagulants. I am in good form and feel a bit like a fraud: surely if everyone is taking this so seriously, I should be in pain?
And suddenly there is talk of a medical evacuation, by air ambulance, to Brussels. The high level of troponins indicated heart damage – a probable heart attack – and I need a coronography, which means that a catheter has to be inserted into my arteries to see what is going on. This can be done in Ghana, but if it results in a need for further intervention, I should be in a place which has all the necessary resources. I rest in my bed, imagining all the administrative procedures that someone out there is handling to organise my departure. My night is uneasy, but I get some sleep.
The next day is spent swallowing frequent medicines and waiting for the air ambulance to arrive from Germany. I ask my husband to pack a case for me: what will I need? How long will I be away? I estimate a week, and keep the list simple: two nightdresses, underwear, a warm set of clothes, shoes, a coat, a washbag. We are fortunate in that we have a fully equipped apartment in Brussels.
I am given a dinner of tough meat which is difficult to swallow, but I decide I need to get something into me as I’m not sure when my next meal will be. Late that evening a doctor and nurse, just arrived from Germany, sweep into the hospital and take control. It feels like a scene from a hospital soap opera. My husband and I are whizzed by ambulance to the airport, where all the departure procedures have been organised in advance.
Am I afraid? More than afraid, I am apprehensive…apprehensive about my ‘to do’ list…
Apart from the doctor and nurse, there’s a paramedic, the pilot, and the co-pilot on the small plane. I am on a narrow bed like a stretcher, hooked up to a blood pressure machine. My husband is on an armchair. I feel as though I am on a conveyor belt, with all the controls out of my reach. There’s nothing for it but to try to relax and go with the flow – to trust that whatever decisions have been taken for me are in my best interest. But I am anxious, and have chest pains. The doctor gives me a spray called Nitrolingual to put under my tongue, but I vomit (all the disgusting stringy tough meat) every time I use it.
Am I afraid? More than afraid, I am apprehensive…apprehensive about my ‘to do’ list…Have I paid my phone bill? Is the TV subscription up to date? Did I leave petty cash in the kitchen? Do we need to buy gas? Who will do all the things I usually do? What about the tickets for the ball next week? And the batik workshop I have half organised for Wednesday?
If I don’t make it, I tell myself, it won’t really affect me, in a sense…I am not a religious person…recently I discovered the writer and psychotherapist Irvin Yalom (Thank you, Barbara Alamberti!) and this quote has remained with me:
‘Life is a spark between two identical voids, the darkness before birth and the one after death.’
If I believe anything, it’s that in death I will simply return to whatever state I was in before I was born, and that will be a completely non-aware state, so it can’t be too traumatic…but what a hassle it will be for everyone else! Nobody knows my passwords, nobody knows all the commitments I have in my head, people will have to start worrying about where to throw my ashes and what music to play at my funeral…no, please, let me make it, at least for a little while, so that I can write handover lists for people and leave things in order.
My mind flashes back a few months when my husband and I were about to go on holiday. ‘If I die tomorrow,’ I told him, ‘I won’t have printed my boarding pass.’
‘Well don’t worry, if that happens, you won’t need it,’ he replied. He’s always telling me that however hard I try, my ‘in’ tray will never be empty.
It’s a strange time: a time for re-evaluating priorities – a time during which the fragility of life becomes blindingly clear.
But I do make it. From my stretcher on the runway at Zaventem airport I act as interpreter between the French-speaking paramedic and my English-speaking Indian doctor from Germany. We are whisked off by ambulance to A&E in St Luc Hospital, where I am settled into a curtained cubicle and my blood pressure is measured every 15 minutes for 6 hours, so there is no hope of getting any sleep. I am not allowed to eat or drink anything – not even a sip of water. Then I am moved to a private room in Intensive Care, where my BP is measured every hour and blood samples are taken every six hours. My body soon starts looking rather bruised. But I am delighted to be offered a meal!
The following day I have my coronography, which is not painful (I ask for a tranquilliser beforehand!) This reveals that I have a pre-existing rare condition called fibromuscular dysplasia (FMD) in my two renal arteries. This is a malformation of the artery walls, and is found most often in women a lot younger than I. The chest pain episodes, I am told, were a type of heart attack called Spontaneous Coronorary Artery Dissections (SCADs).
I am kept in hospital for one more night, then discharged with a prescription for statins, betablockers, cardioaspirin and blood pressure tablets, and a recommendation to take things easy.
 I rest for ten weeks. My husband takes time off work to be with me. We live simply in our Brussels apartment, through a grey Belgian autumn. It’s a strange time: a time for re-evaluating priorities – a time during which the fragility of life becomes blindingly clear. It’s a time during which I feel surprisingly calm, and it’s comforting and comfortable. I have few responsibilities, and enjoy the most basic activities like ironing and cooking. We are clear-headed, and we soon become aware that we have had enough of our amazing roller-coaster professional life: we decide we will pack it all in at Easter.
I rest for ten weeks. My husband takes time off work to be with me. We live simply in our Brussels apartment, through a grey Belgian autumn. It’s a strange time: a time for re-evaluating priorities – a time during which the fragility of life becomes blindingly clear. It’s a time during which I feel surprisingly calm, and it’s comforting and comfortable. I have few responsibilities, and enjoy the most basic activities like ironing and cooking. We are clear-headed, and we soon become aware that we have had enough of our amazing roller-coaster professional life: we decide we will pack it all in at Easter.
A month after my evacuation I have a follow-up appointment with my cardiologist: all seems well, but he refers me to a colleague of his, who specialises in Fibromuscular Dysplasia. I agree to become part of the FMD research pool (you can read more about his work here): perhaps my experience will be able to help others…and on top of that, I find it reassuring to know the experts are keeping tabs on me.
We have a quiet Christmas and New Year, and by early January we are completely rested, and ready to join the family for our son’s wedding by the banks of Loch Lomond: a spectacular venue for a moving and meaningful humanist ceremony. And I shed many many happy and grateful tears.

And now, back in Ghana, I am taking it easy, resting a lot, napping every day, and gently easing back into an exercise routine, swimming and doing yoga regularly. Soon I will have to start facing up to the move: a big move which will mark the end of forty years gallivanting around the world. I will need to stay as calm and focussed as possible.
I have understood that I don’t always need to be in control: I can accept, even embrace, unpredictability, and let go of worries I can do nothing about.
It’s hard to judge how careful to be: it’s estimated that SCADs recur in 10% of sufferers within 10 years, but what do those numbers mean? Will I be one of the 10%? How often are recurrences fatal? At least, if there is a next time, I will recognise the signs…and I have paid most of my bills and left a few handover notes…
In retrospect I see that for well over a year leading up to the evacuation I had been in a permanent state of severe stress. I had been suffering from insomnia, from chronic mouth and throat ulcers, was moody and irritable, and incapable of taking simple decisions. And that state had become my ‘norm’. My forced period of rest has made me aware that life doesn’t need to be complicated; that actually, it’s great to feel relaxed. I have realised that if I wake at four a.m., it’s possible to turn over and go back to sleep for a few hours, rather than getting up and starting to answer emails or do administrative work. I have understood that I don’t always need to be in control: I can accept, even embrace, unpredictability, and let go of worries I can do nothing about. I can even accept that there will always be a few things pending in my ‘in’ tray. Life is much more fun that way.
Let me end with another quote from Yalom, which has become my mantra:
‘Live your life to the fullest; and then, and only then, die.
Don’t leave any unlived life behind.’
So here’s to a life well-lived.
Paola Fornari
Accra, Ghana
January 2018
Photos ©Paola Fornari